Sickle Cell Disease for the Correctional Nurse
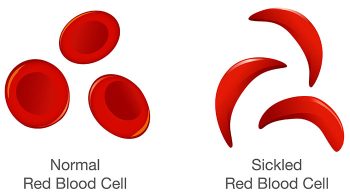
Sickle Cell Disease (SCD) is a group of inherited blood disorders characterized by the presence of abnormal hemoglobin, called hemoglobin S (HbS), in red blood cells. This genetic condition leads to the formation of rigid, sickle-shaped red blood cells that can obstruct blood flow and cause various complications. There are three types of SCD. Understanding the pathophysiology helps to explain why individuals with SCD experience various symptoms and complications. It also guides the development of treatments aimed at preventing sickling, managing symptoms, and reducing complications associated with the disease.
In this class, we will discuss the pathophysiology of Sickle Cell Disease, and its treatment and management. We will also review nursing interventions for the patient with Sickle Cell Disease.